
Every year tens of thousands of spinal cord injury survivors with non-healing pressure wounds lose precious quality of life when they have to go to bed to heal properly. Some die after having been sent home from hospitals with no hope for healing. Some get clinically depressed after years of fighting recurring infections and even choose to die. With modern medicine making encouraging strides in treating many diseases and conditions, why do pressure sores continue to ruin lives?
“The main problem is a wound care system that is fractured in its ability to deliver needed treatments,” says Dr. Bruce Ruben, founder of Encompass Healthcare in West Bloomfield, Mich., a facility that is becoming known for its efficient, compassionate, patient-centered ethic. “Nothing I do is novel,” says Ruben. “The medical treatments I use are typically available, but the problem is they are discontinuous — there is no centralized place delivering everything that is needed.” Ruben and his staff treat people 24/7 from their uniquely equipped facility, even doing home calls for wound dressing, IV infusion and grafting. “My whole career has been about keeping people out of hospitals,” he says.
Although board certified in three specialties — infectious diseases, internal medicine, and undersea and hyperbaric medicine — Ruben insists it is not enough. “The problem is wound care is not a recognized specialty. You can’t be a board certified doctor of wound care.” The result, he says, is there are too many people in the field who are not sufficiently knowledgeable about understanding the root causes of non-healing wounds. When combined with an antiquated delivery system, healing does not happen as it should.
The Road to Learning
Early in his career, Ruben saw the dangers inherent in hospital treatment. “Back in 1990 most patients were inpatients when they got an intravenous antibiotic, and to me that seemed ridiculous. One, they were at risk for getting a hospital-acquired infection, and two, after they got their antibiotic, they just laid around in a hospital bed for another 23 hours. It just didn’t make sense to me.”
He got interested in wound care and asked a vascular surgeon if he could attend hospital rounds with the doctor, nurses, physical and occupational therapists. “I saw different opinions and different ideas, and it didn’t seem that there was any commonality in thinking,” he says. “So I decided I would figure out for myself why wounds didn’t heal.”
In 1994 he began his own infusion therapy practice. Over the next several years he gradually began using other wound care treatment modalities, and by 2005, he had became convinced that what he had learned — combined with his three specialties — put him in a perfect position to practice all-encompassing wound care.
Kitty Carpenter became one of his first staff members in the 1990s. She has seen Ruben’s practice grow and change since then. “We’ve been working together so long, I guess we’re just stuck with each other,” she jokes. “Five years ago he changed his whole train of thought and completely revamped his practice to include and appeal to people with SCI. Just three years ago he gutted out his office and re-did everything to make it wheelchair accessible, right down to the coat racks.”

Not only does his facility have reclining adjustable exam chairs, a Hoyer lift, a small operating room for grafting procedures, a roll-in shower for clean-up if needed, and complete ADA access in every room, patients notice something different about the people who work there. “You go in and they offer you snacks and drinks when you are waiting. It’s not the usual doctor office experience,” says Heather Chabert, 42, a C5-6 quad. “Dr. Ruben is so different than any other doctor I’ve been to. Sometimes I ask myself, ‘Am I in another world?’”
Chabert has had wound grafting done both at the Encompass facility and her home. “He brings everything with him. I’ve never had anything get infected. He’ll have a bag, and the graft comes in a special container. He uses all the blue pads and sterile equipment and gloves, and the bright light they use in the office. And Kitty. She is beyond amazing.”
Grafting is more convenient when done at home, says Chabert. “Doctors have come before, but all they tell you is to put on ointment and a dressing, then it scabs up, has to be debrided, and they don’t do anything else. Dr. Ruben is just so much about us. It is so rare that this happens.”
Other satisfied customers are equally impressed with the care they get. “If you go in the back room,” says Kathy Best, 68, a full-time wheelchair user since 1985 from a progressive birth defect, “there are plaques on the wall, but they’re not his credentials. They’re Most Compassionate Doctor Awards. And his staff is equally as nice.”
Best knows true compassion when she sees it, having experienced the absence of it while spending years in bed with non-healing wounds before coming to Encompass. A doctor she refers to ironically as “Dr. Warm and Fuzzy” had told her she would never heal. “He said I would have to go to a nursing home for the rest of my life.”
Having spent three years in bed, this was more than Best could take. She became very depressed and quit eating, even planned her funeral. “I couldn’t stand the pain in my chest, the sadness. I just wanted to be done with it. My husband said, ‘Please, don’t leave me,’ and then a friend gave me a news article about Dr. Ruben. It was a spiritual thing, a Godsend.”
Best says she was down to 80-90 pounds when she went to Encompass with wounds on both ischials. “No stone was unturned. They put me on a picc line, and he has me on total protein nutrition. It has been a couple of months now. I’ve gained weight, I’m definitely healthy again, about 115 pounds. Everybody is remarking on it. He treats the whole person, definitely, he does.”
On the day she was interviewed, with one wound closed and hope regained, Best had an appointment the next day in Pittsburgh for flap surgery to close the second wound. “My goal is to go to the mall. I sometimes think the economy is bad because I haven’t been there in so long.”
Hyperbarics and Protein
Michael Beach, 40, of Monroe, Mich., a T9-12 complete para since 2007, began having pressure sore problems sometime in 2009. “It started with my coccyx and spread to both ischial areas,” he says. For the next three years, he was shuttled from one doctor to another and multiple hospitals. Three different doctors told him they could do nothing more for him. Then his father-in-law gave him a news article about Ruben and his facility. “I gave it to my nurse, who called him, then told me, ‘We’ve got to go see this doctor.’ We got to Dr. Ruben’s office and he said, ‘I can help. It will take time, but I can help.”
Bone infection was preventing healing, so Ruben started Beach on IV infusion and hyperbaric treatments. “I had 90 hyperbaric treatments over about a year, with three months off,” says Beach. “He set me up to do IV therapy at home. Everything worked fine. With a picc line and infusion bottles, it took one hour per day. I did it myself. A nurse showed me how.”
A third leg of Beach’s treatment was nutritional therapy, a special emphasis that Ruben feels is too-often neglected in wound care. “It was all by mouth, no pills,” says Beach. He ate a prescribed diet of 2,000 calories during the day, then got another 2,000 calories each night with tube feeding. Ruben used a calorimeter to determine Beach’s nutritional needs for healing, with a special emphasis on protein.
One year after coming to Encompass, after healing had progressed significantly, Beach was referred to the University of Pittsburgh Medical Center for surgery to close the wounds. “The doctor he sent me to was able to move the muscle around and closed all three wounds in one operation,” says Beach. “And he didn’t need to do flap surgery.” He was discharged and went home five weeks earlier than expected. Now he’s on a Clinitron air-fluidized bed for three weeks to make sure the wounds heal completely and stay closed.
Fighting Insurance, Ineffective Doctors
Robert Gress was 48 in 1986 when a wall fell on him at work, paralyzing him at the T12-L1 level. He came from a big family and was very active, even after his injury. “I hunted the next 10 years with no problems. Never had any sores or anything. Rolled through the woods, had a blind made of cloth, threw it over my shoulder, set it up.”
He developed a wound on his heel in 1996. Two years later he accidentally sat on a toy, causing a wound on his butt. They both healed. Then in 2006 he got a cellulitis infection from a sore on his outer malleolus (ankle bone). “I got in the bath and my leg was three times its normal size. I went to emergency and sores popped out on the side of the leg. They sent me to wound care, but the doctor never got within five feet of me. All they did was suggest a wound vac.”

Gress decided against the wound vac and instead went to see Ruben. He, too, had seen one of the three articles about the doctor whose specialty was healing wounds that wouldn’t heal. “He said it smelled bad, probably had a bone infection, so he took a culture. Then he started me on IV infusion and hyperbarics.” What followed was a rollercoaster battle with his workman’s comp insurance that went on for years. “They sent me to four other doctors, but none disagreed with what Dr. Ruben was doing. They kept sending me to other doctors because they couldn’t get one to disagree.”
In a nutshell, his insurance company didn’t want to pay for expensive hyperbaric therapy, among other things. Ruben got involved on Gress’s behalf, and a lawsuit followed. “Dr. Ruben got their records, and in one paragraph it said, ‘The only way we will see an end to payments is on his [Gress’s] demise.’”
Gress’s wounds have healed more than once, but have a tendency to recur. Edema has been a persistent enemy of healing. His latest treatment, venous ablation [see sidebar], has improved healing by re-routing return blood flow and providing a more efficient way to drain off excess fluids.
Now, if he can get his insurance to pay for a power chair with tilt-in-space, he hopes to remain wound-free. In the meantime, he gets his care at home. “Dr. Ruben is just a caring person. He comes out to my house, he sends nurses, he re-did his whole office for wheelchair users. People say doctors don’t come to your house anymore. I tell them, ‘Oh yes they do. This one does.’”
• Encompass Healthcare, 2300 Haggerty Road, Suite 1190, West Bloomfield Township, MI 48323, 248/624-9800; www.encompasshealthcare.com
Understanding Wound Healing
Dr. Bruce Ruben of Encompass Healthcare says, “Malnutrition [protein deficiency] is probably the most common reason I see why wounds won’t heal.” According to him, there are five main reasons why a wound doesn’t heal:
• Pressure
• Infection
• Edema
• Impaired circulation
• Poor nutrition
“You need to evaluate these all at one time,” says Ruben, “because if any one of the five has not been evaluated and managed, no matter what you are doing with the other four, you are still not going to accomplish healing.”
Here is a listing of terms that are important to understanding wound healing, organized according to their relationship with each other:
Repetitive trauma. Pressure from sitting, lying, bumping, scraping or bruising.
Decubitis ulcer. A skin breakdown caused by repetitive pressure.
Cellulitis. Skin infection that begins in a localized area and spreads. More common in lower extremities, where swelling (edema) often occurs.
Osteomyelitis. Bone infection. The most difficult type of infection to overcome for wound healing.
IV infusion. Intravenous infusion of an antibiotic. Can happen in a hospital, an outpatient clinic, or with a picc line, at home.
Picc line (Peripherally Inserted Central Catheter). A small catheter with an elongated line that is implanted in an arm vein for easy hook-up when longer term (up to six weeks) IV infusion is needed.
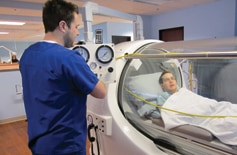
Hyperbaric chamber. A closed chamber that increases the pressure of oxygen by a factor of 10. Used mainly when wounds won’t heal due to bone infection.
Edema. Swelling due to accumulation of fluids and/or infection. Can bring on infection and/or inhibit healing.
Manual lymphatic drainage. Massage by a trained technician to move fluids accumulating below the skin and soft tissue back into the blood vessels. Decreases edema.
Sequential compression device. Much like an elongated blood pressure cuff. A device that alternates inflation and deflation sequentially and pushes fluids and blood upwards. Decreases edema.
Venous return system. The system of veins that transports blood back to the heart. Most important in lower extremities. Spinal cord injury often disables this system since muscle contraction, which activates it, has been lost.
MRV — Magnetic Resonance Vein Imagery. An MRI that enhances evaluation of the venous return system.
Venous stasis. A condition where blood no longer effectively returns to the heart since it is static in the veins. Blood and fluid leak, accumulating in soft tissue, causing edema and red staining to the skin.
Venous ulcer. A skin breakdown that occurs when venous stasis, severe cellulitis or both are present. Blood and water blisters appear, followed by skin breakdown.
Venous ablation. A radio frequency technique for ablating (cauterizing) malfunctioning veins, thereby causing blood to seek another return route.
Arterial circulation. The system of arteries that delivers blood from the heart pumping to the entire body. It is pressure dependent.
Venous circulation. The system of veins that returns blood to the lungs for oxygen and on to the heart. It is volume dependent. Gravity can work for or against this circulatory system depending on if the vein is above or below the heart.
Peripheral artery disease. When peripheral arteries in the legs become clogged with plaque, inhibiting or blocking blood flow.
Transcutaneous oximeter. A device that determines the amount of oxygen that blood delivers to a wound area.
Pre-albumin. A marker that indicates the level of protein in blood. The first step in determining whether sufficient protein is available to heal wounds.
Protein deficiency. For wound healing, tissue building and functional maintenance, protein is the most important building block in the body. A deficiency prevents healing (analogy: a house needs to be framed before it can be bricked).
Indirect calorimetry. A method of determining the body’s total nutritional needs if one were at complete rest. Calculates the basal metabolic rate. Additional calories are required above this rate to heal wounds.
Catabolic state. When a body is severely malnourished. To get protein and additional calories for survival, the body “cannibalizes” itself (breaks down muscle and tissue).



Recent Comments
Abdul Mansour on Testing Two New Seat Designs That Will Let You Fly in Your Wheelchair
Alejandra on Adaptive Products Roundup: May 2026
Lisa Blinn on A Malpractice Case Against ParkingMD