

LT is a difficult, sometimes fuzzy-edged scientific adventure, not a predictable task like learning to play Wii dodge ball with the kids.
When I first dropped by the Next Step Fitness Center, situated in a nondescript mini-mall in the Los Angeles suburb of Lawndale, Janne Kouri had been walking, or more precisely, stepping, with a walker for about two weeks. Three years ago Kouri, now 34, was playing volleyball on the beach and decided to dive into the ocean, hitting a sandbar and ending up a with a C5-6 incomplete SCI. In that stark nanosecond many paralyzed people have experienced, Kouri went from a former 280-pound defensive lineman at Georgetown to an immobile tetraplegic.
Kouri eventually hooked up with a program called the NeuroRecovery Network and a rehabilitative research doctor at Frazier Rehab Institute in Louisville, Ky., named Susan Harkema. Harkema, a muscle biochemist by training, had been a post-graduate fellow in the mid-90s at UCLA when a group of research physiologists and neurologists, in particular, Drs. Reggie Edgerton and Bruce Dobkin, were conducting the first experiments in what has come to be known as “locomotor training.” The lineage of this new chapter in rehab is that short and direct — from a laboratory at UCLA, through Harkema in Louisville, to Janne Kouri stepping with a walker in Lawndale.
Kouri’s not the only poster crip for LT these days. He’s one of about 270 now being tracked by NRN, which was founded by the Christopher and Dana Reeve Foundation and is operated principally through seven major rehab institutes across the country, including Frazier, Kessler in New Jersey, the Boston Medical Center in Boston, and facilities in Ohio, Atlanta, Houston and Philadelphia. Predicated on the belief that there needs to be rigorously monitored, sustained empirical evidence about the effects of LT training, the NRN is well beyond the anecdotal phase and heavy into precise results. They want to get to the bottom of what some have deemed damn near a miracle cure for people with SCI who want to walk, and others see it, to quote one prominent researcher, as “a bit of false hope.”
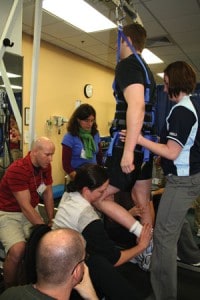
So, what exactly is “locomotor training”? You may have heard about it in vague, glowing terms — “people learn to walk again” — and dismissed it as too good to be true. First of all, it’s a contraption: a treadmill and a full body harness, all calibrated and controlled by a computer program operated by a trainer. Aided by three or four other trainers, the subject is strapped into the harness and his paralyzed legs, at calculated degrees of weight-bearing, are guided to simulate repetitive walking on the treadmill. Do this long and hard enough, with the proper input and guidance from the trainers — very important — and you too might end up stepping across a room like Kouri.
Or not.
LT is a difficult, sometimes fuzzy-edged scientific adventure, not a predictable task like learning to play Wii dodge ball with the kids. The science begins with a simple, elegant theory — that the spine doesn’t need the brain to learn to walk. Edgerton started working with animals around this idea as far back as 1976, and, as Dobkin explains his findings, “they pointed to mechanisms in the spinal cord called ‘special pattern generators,'” which, through a complex set of reflexes, could initiate walking without input from the brain. As another key researcher, Dr. Andrea Behrman, director of the Locomotor Training and Recovery Research Program at the University of Florida, puts it: “LT is the attempt to give the sensory experience of walking to try and drive the motor output of walking.” Through precise feedback and learning, called cueing, the subject tries to engage these mechanisms, using his own brainpower, to make the response volitional. Part one: the spinal cord creates new motor patterns for walking. Part two: you tell those impulses what to do. End result: walking over ground.
Who’s In and Who’s Out?
In ongoing experiments over the last 18 years, LT researchers have discovered, not surprisingly, that functional stepping is a difficult thing to pull off, and that it doesn’t quite work with everyone. And even if it does work, it might not help any more than conventional rehab protocols. In a trial by Dobkin and others published in the Journal of Neurology (SCILT study, 2006), the multisite research team found people with incomplete injuries admitted for rehab within eight weeks of onset profited equally from both LT and traditional over-ground mobility therapy. “Both groups,” Dobkin says, “improved equally well and improved quite a bit. In the end, 90 percent of all subjects could walk over ground.”
(Incomplete injuries, as defined by the American Spinal Injury Association are rated B — sensory but no motor function; C — incomplete motor function; and D — more incomplete motor function than C. Complete injuries are rated A — complete absence of motor or sensory function).
Dobkin’s SCILT study aside, researchers like Edgerton and Harkema see tremendous potential in LT and weight bearing. “When you stand up (bear weight), your whole physiology changes,” says Edgerton. “Every animal organism on earth has evolved in a One G (earth gravity) environment. Our physiology is built to work in this environment.”
For some, LT might not only help you stand and walk, it could also create big changes in all kinds of body functions, such as balance, blood pressure, bowel function, bone density, glucose tolerance (think Type 2 diabetes) and of course, strength. As Kouri says after his long course of training, “My blood pressure has improved dramatically, my circulation has improved dramatically, plus my muscle tone and my overall well-being.”
That’s all well and good, but who can achieve these benefits? Edgerton doesn’t mince words. “I think it’s very clear — extremely clear — that individuals with an incomplete SCI have a very high chance of being able to recover effective stepping.” That means, in essence, those who have been designated ASIA C and D. Apparently, you need to have some motor or sensory response going in to help generate the new patterns in your spinal pattern generator. That might be some actual leg or trunk movement, but it could also be spasticity or hyper-reflexia. In Behrman’s words, “Somehow, somewhere, some circuit [must be] intact. Someone with a complete spinal cord injury — that’s a harder row to hoe.”
The candidate pool for LT, depending on who you talk to, could be large or small. Some say that over half of all SCIs these days are incompletes. If the recent Reeve Foundation paralysis census is even close — 1.275 million SCIs in the United States — that’s a hell of a lot of incompletes who might benefit. On the other hand, “incomplete” — despite the letter gradations — is a big, broad, inexact category. To be precise, more data is needed. That’s what the NRN, among other ongoing research projects, is all about.
Dobkin doesn’t see the pool as all that large. If you factor out the completes on one end of the spectrum and the barely-incompletes on the other (already halfway to walking), who’s left? “It leaves,” says Dobkin, “the lower-level ASIA C person who has a little bit of movement and can maybe flex slightly at the hip or extend the knee or put some weight into the knee … it’s interesting, but there aren’t a lot of people like that.”
Expectations Are Key
Harkema thinks that limiting LT access to strict ASIA categories may be premature. But let’s say you have an incomplete injury and sign up. What’s involved? First, a lot of strenuous work, like training for a marathon, only harder. Alex Pass, an 18-year-old C6-7 incomplete, works out three times a week on the LT device at Next Step. You can watch the sweat pour off him as he tries to plant one foot in front of another. He’s been at it for nine months, not a long time by LT standards. Kouri has been at it for two years and nine months, four sessions a week, an hour a session. That’s an enormous commitment of time and energy. And sheer will. Pass was a former wrestler. Kouri once made 16 quarterback sacks in one season. You don’t have to have an athletic mindset going in — Harkema works with people from grade school to 60 — but you certainly need motivation.
Kouri’s dedication extends far beyond training. He and his wife, Susan, actually founded Next Step as a nonprofit fitness center for people with physical disabilities. Some clients go there for general fitness at cut rates ($75 a month). Thirteen are enrolled in the LT program, which is all they can handle at one time. Funded by friends and family, the people at Next Step are trying to create a low-cost, accessible model for many such public centers to come.
For most of us, the main question remains: Is it worth it? Harkema compares the results and reactions of two participants. Participant number one could never walk, no matter what (ASIA A), but after LT, he could stand with a walker for as long as he wanted. As Harkema says, “I was just blown away but he was not happy — he wanted to walk.” Participant number two, another complete, pursuing the same course, ended up being able to stand for only two or three minutes. For him, this was an absolute life-changer. He was thrilled. He could stand up to get into a car. It made a huge impact on his life. The difference between the two: expectations.
Dobkin’s own brother, Craig, a teacher in Colorado, sustained an L1 injury while rock climbing and was one of the first human guinea pigs to mount the LT treadmill back in the mid-’90s. He helped design the first harness, using his knowledge of mountain climbing apparatus. Within 10 minutes, Dobkin says, Craig started to regain movement, and within a week or so he could traverse a room on crutches. Today, about 15 years later, he continues to walk only a few steps on crutches and spends 90 percent of his day in a chair. But it has changed his life. “Standing itself made me cry,” he says, and he sees his slow-walking as a gift. “It changed me both psychologically and physiologically. To walk on crutches, you have to be strong. I do it every day.”
“Making incremental changes in peoples’ lives,” Harkema says, “has been the biggest achievement.”
You may be fully eligible for this form of neuromuscular re-education but may not have the laser-like drive or optimism of a Kouri or a Craig Dobkin. The cost/benefit ratio of applying that much time and energy to walk 20 feet in a minute-and-a-half versus rolling the same distance in three seconds may not add up. Since no one at this point can say with absolute certainty how any individual will respond, you are taking two leaps of faith at once: one, that you’ll improve, and two, that the improvement will make a real difference in your life.
True Cost Versus Benefit
The seven NRN rehab centers have such standing that many forms of conventional health insurance plans are billable for LT. There are two community-based fitness centers associated with the NRN — one is in Louisville and the other is Next Step. Insurance in this setting is much iffier, though Christel Mitrovich, the director of Next Step, has received reimbursement in one early claim. Otherwise, you’re on your own — and it can be pricy. Next Step charges a monthly fee of $1,100 for LT training, and that hardly covers their direct costs. There’s the shop, the machine, the data collecting and four or five trainers every time you climb up on the rig.
So, will locomotor training get the whole paralyzed world walking again? No. Is it much ado about nothing? No. It’s probably much ado about something and that something depends on the state of your injury, your dedication to a strenuous, potentially frustrating course of action, your contact with people who know what they’re doing, and your expectations. As Edgerton says, “I think I sometimes come off like I’m trying to sell something. Our objective really is to determine what works best. I want a physician to be able to look an SCI in the eye and say, ‘OK, this is what we know, this is the probability of what could happen, and these are your options.'”
This is science, after all, not dogma. It evolves, changes, backtracks and runs into dead ends. And it takes time. Asked why it is taking so long to have definitive answers about this training, Harkema says it is in part because “scientists and clinicians don’t have a clear communication bridge.” Plus, she says, “there is a misperception that you buy some equipment, put some people in a harness, move their legs, and something happens. It’s much, much more complicated than that.”
Janne Kouri, for one, is pretty sure what his benefit will be relative to his cost. “I absolutely think I will be able to walk functionally one day with the help of a walker or some other device. And not just in the gym. In my daily life.” Check out the YouTube video called, appropriately, “Janne’s First Days Stepping with a Walker” — seriously, go watch it — and you might be hard-pressed to curtly dismiss his optimism.
For More Info:
• NeuroRecovery Network, Reeve Foundation, www.christopherreeve.org
• Next Step Fitness, www.nextstepfitness.org
• Janne Kouri on YouTube, www.youtube.com/watch?v=RnrfgZhjlSg
Support New MobilityWait! Before you wander off to other parts of the internet, please consider supporting New Mobility. For more than three decades, New Mobility has published groundbreaking content for active wheelchair users. We share practical advice from wheelchair users across the country, review life-changing technology and demand equity in healthcare, travel and all facets of life. But none of this is cheap, easy or profitable. Your support helps us give wheelchair users the resources to build a fulfilling life. |


Recent Comments
Bill on LapStacker Relaunches Wheelchair Carrying System
Phillip Gossett on Functional Fitness: How To Make Your Transfers Easier
Kevin Hoy on TiLite Releases Its First Carbon Fiber Wheelchair